What is osteoporosis?
Osteoporosis is the “thinning of bones” . It causes bones to become weak and fragile with an increased susceptibility to fracture, meaning that a minor fall or stress can cause a fracture. This is because the bones are porous like a sponge so are easily compressible. Osteoporosis-related fractures most commonly occur in the hip, wrist and spine and can result in disability.

Bone is living tissue that is renewed constantly, if the creation of new bone doesn’t match the breaking down of old bone then osteoporosis occurs. As we age, bone mass is lost faster than it’s created. Therefore creating a bone mass in your youth will help you in your old age.
What are the symptoms?
In the early stages of bone loss there are no specific symptoms therefore calling it the “ silent disease”. But once bones have been weakened, these symptoms may appear including:
- Back pain
- Height loss and hunched postrure
- A bone fracture
Who is at risk?
Osteoporosis affects both men and women, as they get older, though women are much more likely to develop osteoporosis, white and Asian women having the highest risk. Family history and body frame do put you at greater risk, a smaller body frame giving you less bone mass as you age.
Hormone levels that are too much or too little have a connection with being osteoporotic. Examples of these hormones are:
- Estrogen: Estrogen levels decrease at menopause and during cancer treatments.
- Testosterone: Men experience a gradual reduction in testosterone levels as they age and due to treatments for prostate cancer.
- Thyroid Hormone: Thyroid hormone or thyroid medication can cause bone loss.
Other hormones: Osteoporosis is also connected with overactive parathyroid and adrenal glands.
Low calcium intake, eating disorders and gastrointestinal surgery contribute to lessening of the bone density due to improper food intake. Nutrition and osteoporosis are closely linked. You must get the right nutrient in your diet or through supplements.
Steroids and other medication interfere with the bone-rebuilding process.
Sedentary lifestyle. Weight-bearing exercise and activities like walking are beneficial for your bones. People with an inactive lifestyle have increased risk of osteoporosis.
Excessive alcohol consumption increases your risk of osteoporosis.
Tobacco intake contributes to weak bones.
How so I test for osteoporosis?
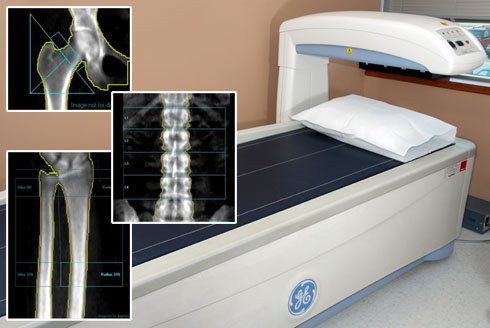
By the time X-rays can detect osteoporosis, at least 30% of the bone has already been lost so bone density testing , called DXA or DEXA, is recommended for all women after menopause. This screening procedure is painless and checks the hip wrist and spine bone density as they are the areas most affected by osteoporosis. The test takes only five to 15 minutes to perform and exposes patients to very little radiation. The machine uses low levels of X-rays to determine the proportion of mineral in your bones. A bone mineral density test is another way to check your bone health.

What is the treatment for osteoporosis?
None of the treatments for osteoporosis are complete cures. Although there are medications to improve the strength It is difficult to completely rebuild bone that has been weakened by osteoporosis. Therefore, prevention of osteoporosis is as important as treatment.
If the risk of osteoporosis is not high, treatment might not include medication and might focus on lifestyle and modifying risk factors for bone loss. Osteoporosis treatments is referred to as the “basic CDE’s” — calcium (C), vitamin D (D), weight-bearing exercise (E).
Exercise is important in both the prevention and treatment of osteoporosis. starting a regular exercise program may help prevent further bone loss. You can change your exercise habits to improve your current state of osteoporosis. It is important to avoid exercises that can injure already weakened bones, so it is best to discuss discuss your exercise options with your doctor .